What is Mooren’s ulcer
Mooren’s ulcer (chronic serpiginous or rodent ulcer) is a severe inflammatory peripheral ulcerative keratitis.
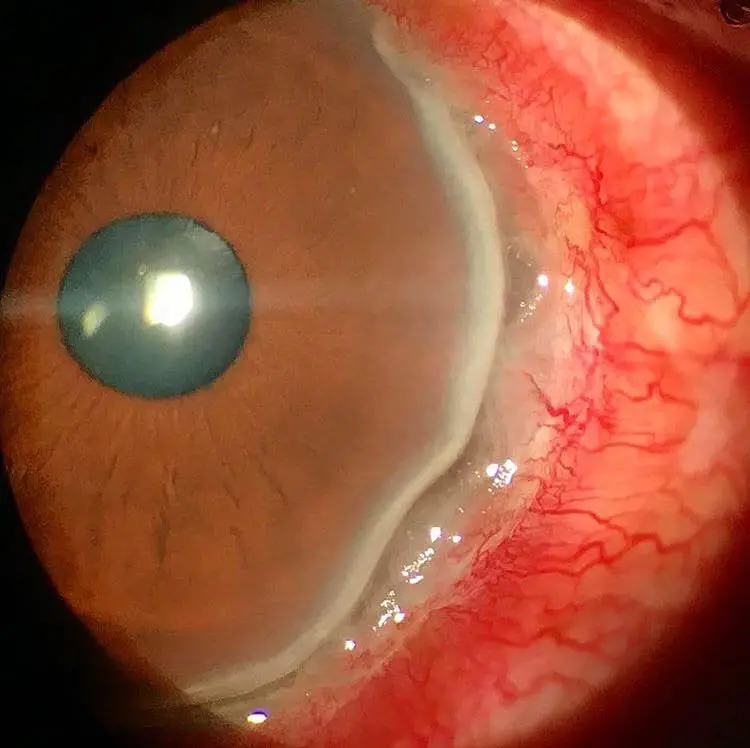
Mooren’s corneal ulcer
Corneal changes in Mooren’s ulcer begin within 2-3 mm from the limbus, first appearing as grey swellings that rapidly furrow, affecting the superficial one-third of the cornea and then proceeding circumferentially and centrally over 4-12 months. The bed of the furrow becomes vascularized, with vessels advancing into the base of the undermined edges of the ulcers.
Mooren’s ulcer cause: Etiology of Mooren’s ulcer
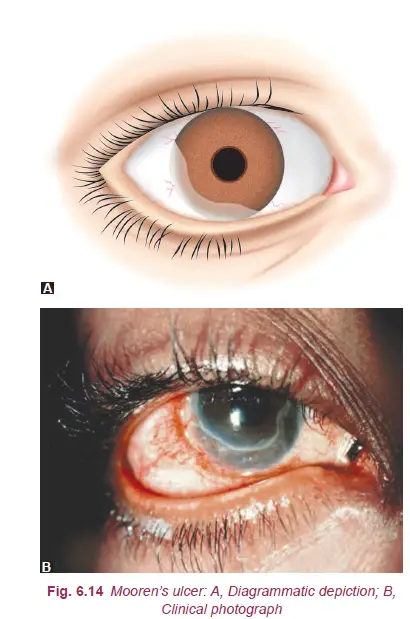
Exact etiology is not known. Most probably it is an autoimmune disease.
see eye disease
Clinical features
Two clinical varieties of Mooren’s ulcer have been recognised.
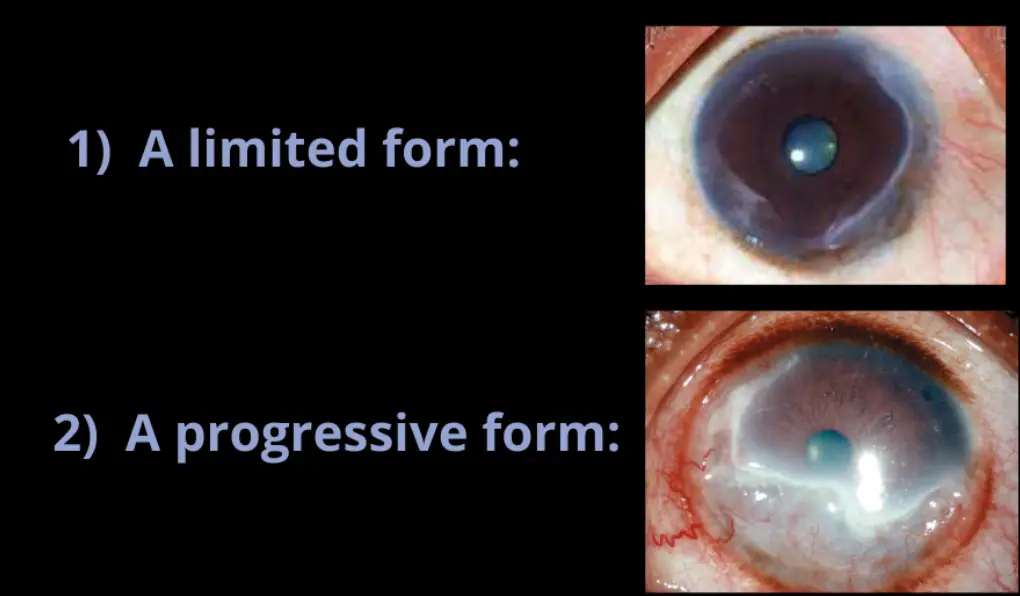
- Benign or limited form which is usually unilateral, affects the elderly Caucasians and is characterised by a relative slow progress.
- Virulent type also called the progressive form is bilateral, more often occurs in young African patients. The ulcer is rapidly progressive with a high incidence of scleral involvement.
Mooren’s ulcer symptoms
These include severe pain, photophobia, lacrimation and defective vision.
Signs of Mooren’s ulcer
• It is a superficial ulcer which starts at the corneal margin as patches of grey infiltrates which coalesce to form a shallow furrow over the whole cornea.
• Peripheral ulcer is associated with undermining of the epithelium and superficial stromal lamellae at the advancing border which forms a characteristic whitish overhanging edge. Base of the ulcer soon becomes vascularized. The spread may be selflimiting or progressive.
• At the end-stage, the cornea is thinned and conjunctivalised.
• Ulcer rarely perforates and the sclera remains uninvolved.
Mooren’s ulcer treatment
Since exact etiology is still unknown, its treatmentis highly unsatisfactory. Following measures may be tried:
- Topical corticosteroids instilled every 2–3 hours are tried as initial therapy with limited success.
- Immunosuppressive therapy with systemicsteroids may be of help. Immunosuppression with cyclosporin or other cytotoxic agents may be quite useful in virulent type of disease.
- Soft contact lenses have also been used with some relief in pain
mooren ulcer vs puk
Mooren ulcer is a severe inflammatory peripheral ulcerative keratitis.(PUK)
Causes of PUK
Peripheral corneal ulceration and/or melting of corneal tissue is not of infrequent occurrence in patients suffering from connective tissue diseases such as:
• Rheumatoid arthritis,
• Systemic lupus erythematosus (SLE),
• Polyarteritis nodosa, and
• Wegener’s granulomatosis.
Distinguishing Clinical features of PUK
• Peripheral acute corneal ulceration with rapid progression, usually in one sector, associated with inflammation at the limbus in one or both eyes.
• Peripheral corneal guttering or thinning may involve entire corneal periphery (contact lens cornea).
• Peripheral corneal melting may result in descemetocele formation or even perforation.
• Corneal ulceration may be the first manifestation of the systemic disease and there may be associated systemic features of any of the causative disease.
Peripheral Ulcerative Keratitis (PUK):
![]() PUK may precede or follow the onset of systemic features. Severe peripheral corneal infiltration, ulceration or thinning unexplained by evident ocular disease should prompt investigation for a (potentially life-threatening) systemic collagen vascular disorder.
PUK may precede or follow the onset of systemic features. Severe peripheral corneal infiltration, ulceration or thinning unexplained by evident ocular disease should prompt investigation for a (potentially life-threatening) systemic collagen vascular disorder.
![]() Clinical features:
Clinical features:
![]() Crescentic ulceration with an epithelial defect, thinning and stromal infiltration at the limbus. Spread is circumferential and occasionally central. In contrast to Mooren ulcer, extension into the sclera may occur.
Crescentic ulceration with an epithelial defect, thinning and stromal infiltration at the limbus. Spread is circumferential and occasionally central. In contrast to Mooren ulcer, extension into the sclera may occur.
![]() Limbitis, episcleritis or scleritis are usually present. As with a Mooren ulcer, there is no separation between the ulcerative process and the limbus.
Limbitis, episcleritis or scleritis are usually present. As with a Mooren ulcer, there is no separation between the ulcerative process and the limbus.
![]() Advanced disease may result in a ‘contact lens’ cornea or perforation
Advanced disease may result in a ‘contact lens’ cornea or perforation
REf : eyewiki.org, AK khurana
Discover more from An Eye Care Blog
Subscribe to get the latest posts sent to your email.


You must be logged in to post a comment.