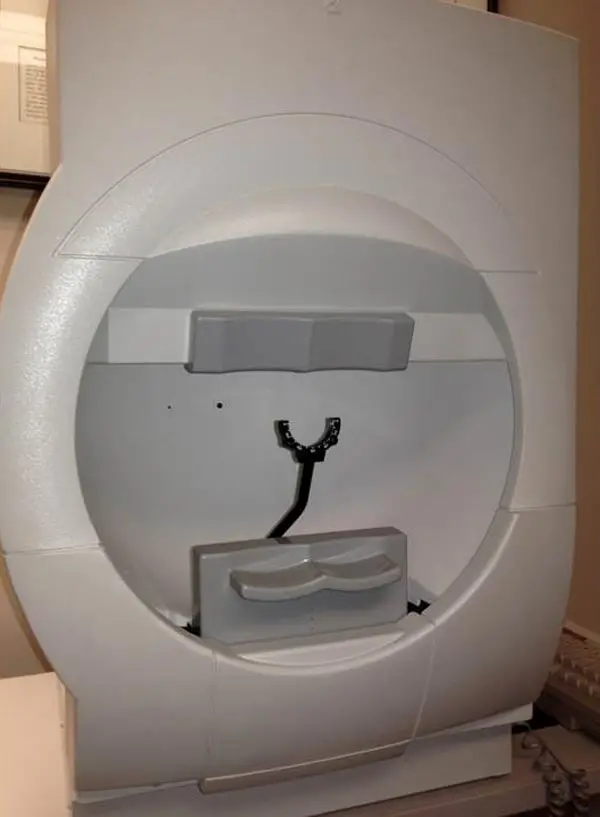
humphrey visual field analyzer
How to Perform Humphrey visual field test?
Several basic conditions must be met for a successful map of the visual field to be produced by any method. The individual must be able to maintain a constant gaze toward a fixed location for several minutes.
Each eye is tested separately while the opposite eye is covered with a patch. Refractive correction must be made with a test lens. Spectacles must not be worn because they can cause false defects in the visual field due to their shape
In addition, correction must be made for presbyopia, to reduce accommodative strain. Standard adjustments for presbyopia are available based on age alone. To correct an astigmatism >0.75 diopters, a cylindrical lens must be used. If the eyelid or lashes obstruct the visual axis, the lid may be taped to the forehead to lift it out of the way.
During Humphrey Visual Field (HVF) testing, the patient places his head in the chinrest and fixes his gaze toward a central fixation point in a large, white bowl. As stated above, this test is an example of static perimetry. It assesses the ability to see a non-mobile stimulus which remains for a brief moment (200 ms) in the visual field.
When the patient sees a presented stimulus, he presses the button on a handheld remote control. Different locations within a given region of the visual field are tested until the threshold, or the stimulus intensity seen 50% of the time, is seen at each test location.
Stimuli vary in size and luminous intensity. Goldmann size III (about ½ degree in diameter) is generally used, but Goldmann size V (approximately 2 degrees in diameter) is available for patients with decreased visual acuity (< 20/200) or other visual impairment. Goldmann sizes I, II, and III are rarely used clinically.
The luminous intensity of the stimuli can be varied over a range of 0.08 to 10,000 apostilbs (asb). It is reported in decibels (dB) of attenuation, or dimming, extending from 0 dB (the brightest, unattenuated stimulus) to 51 dB (the dimmest, maximally attenuated stimulus). If the patient is unable to see even the brightest, unattenuated stimlulus, it is reported as <0 dB.
The Swedish Interactive Thresholding Algorithm (SITA) is frequently used. SITA is a forecasting procedure that uses Bayesian statistical properties that is similar to the methods used for providing weather information and predictions. SITA allows for more rapid analysis than would be possible without forecasting. By taking into account a user’s results in nearby locations, stimuli that are unlikely to be seen, or extremely likely to be seen are not tested exhaustively. Instead the stimuli that are likely near threshold are tested.
Reading the Humphrey visual field test printout.
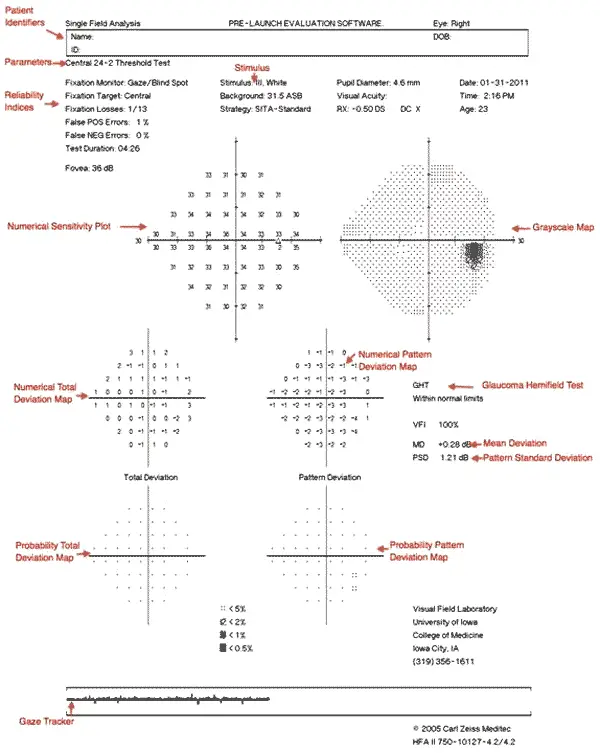
Humphrey visual field test printout can be divided into eight zones for ease of understanding
Zone 1: This section consists of the patient’s information like the patient’s name, date of birth, visual acuity, the refractive correction used for the patient for doing the test, and the patient’s pupil size
Zone 2: This zone mentions the foveal threshold and the reliability indices. The foveal threshold should correspond to the visual acuity of the patient. A good visual acuity with a less foveal threshold would indicate damage to the fovea, and a poor visual acuity with a good foveal threshold would indicate a refractive error that has not been corrected before performing the test.
Zone 3: The greyscale graph is a color-coded representation of the retinal sensitivity of the patient. It is not used for the final interpretation of the field test but is important for patient education. The values closer to 0 dB are illustrated as black points of varying shades, whereas points close to 50 dB are illustrated as white points. The points with sensitivity greater than 40 dB are seen as white scotomas on the greyscale and require careful interpretation. They usually indicate a “trigger happy” patient who has responded without seeing the stimulus (false positive).
The greyscale is useful when comparing the fields of a patient on follow-up. It indicates the progression of the visual field both in extent and in-depth over time at a glance, given the reliability indices are within normal limits.
Zone 4: This zone comprises the total deviation numerical plot and total deviation probability plot. The total deviation numerical plot indicates the depth of the field defect. It compares the dB value of the patient at all the retinal points tested to the normative data stored in the machine for that particular age. The normative database is calculated by collecting responses from a group ofhealthy subjects. The upper 95% of these values are arbitrarily taken as normal, and the lower 5% are considered abnormal.
Zone 5: This zone comprises the pattern deviation numerical plot and the pattern deviation probability plot. These demonstrate the presence of localized field defects and their pattern. To calculate the numerical values of the pattern deviation numerical plot, the values on the total numerical plot are chronologically arranged, and the 7th best point on this data is noted.
Zone 6: This zone consists Of the global indices, which are the mean deviation, pattern standard deviation, the visual field index, and p-value
Zone 7: This consists of the glaucoma hemifield test (GHT). Glaucoma affects the retinal ganglion cells on either side of the horizontal meridian. Therefore, five areas, with a set of retinal points in each area, are tested on both sides of the horizontal meridian and compared. The results are displayed as GHT within normal limits, GHT borderline, or GHT outside
normal limits.
If a single cluster pair differs P value <0.5% or all cluster pair differs P value <1%, machine flags the same as OUTSIDE NORMAL LIMIT. If the P value of hemifield differs by <3%, the machine flags it as BORDERLINE.
Zone 8: It is the raw data collected by the machine and consists of the retinal sensitivity (dB values) of each point tested for that program. Absolute scotoma is indicated by a zero dB value.
Zone 9 : GAZE TRACKING
In most Humphrey perimeters, an automatic dual-variable gaze tracker measures gaze direction every time a stimulus is presented. On the gaze tracking record, lines extending upward indicate the amount of gaze error during each stimulus presentation, with full scale
indicating gaze errors of 100 or more. Lines extending downward indicate the unsuccessful measurement of gaze direction, for instance, because Of a blink.
Humphrey visual field test interpretation

All of the information provided on the visual field printout is important. Patient identity information and the specific test and stimulus size are located near the top of the analysis. It is important to verify that the patient’s birthdate was properly entered as an error will result in comparisons with normals in the wrong age group.
Beneath the patient’s name is a statement giving information about the testing parameters, such as “Central 24-2 Threshold Test.” The first statement, “Central 24” indicates that the central 24 degrees of visual field were analyzed. The next number indicates how the grid of points is aligned to the visual axis.
The number “1” indicates that the middle points are overlying the horizontal and vertical meridians. The number “2” indicates that the grid of points straddles these meridians. This is the setting most commonly used, as it is easier to assess whether visual field defects respect the horizontal or vertical midline.
Next on the report are the reliability indices, including fixation losses, false positives, and false negatives. Fixation losses occur when the patient reports seeing a stimulus that is presented in the predicted area of the physiologic blind spot. False positives occur when a patient presses the button when no stimulus is presented.
Eager-to-please participants sometimes struggle with high false positive rates (i.e., they are “trigger happy”). False positives can often be corrected by providing a simple statement that many stimuli will not be seen even with normal vision. False negatives occur when a patient fails to see a significantly brighter stimulus at a location than was previously seen. False negatives are usually the result of attention lapses or fatigue and are difficult to correct.
The visual threshold is the intensity of stimulus seen 50% of the time at each location. The threshold values of each tested point are listed in decibels in the sensitivity plot. Higher numbers mean the patient was able to see a more attenuated light, and thus has more sensitive vision at that location. To the right of the numerical sensitivity plot is the grayscale map. This map presents sensitivity across the patient’s visual field with lighter regions indicating higher sensitivity and darker regions reflecting lower sensitivity. The sensitivities are not compared to any normative database.
Therefore the map may draw attention to an irregularity within a field, but may minimize field loss if loss is more homogenous across the field. Caution should be used as it can be misleading based on where the machine chooses to make the cutoff between the different shades of gray. The raw threshold data should always be assessed in conjunction with the grayscale representation.
The numerical total deviation map compares the patient’s visual sensitivity to an average normal individual of the same age. It is useful to compare with age-matched normal thresholds as sensitivity normally decreases gradually with age.
Positive values represent areas of the field where the patient can see dimmer stimuli than the average individual of that age. Negative values represent decreased sensitivity from normal.
The numerical pattern deviation map shows discrepancies within a patient’s visual field by correcting for generalized decreases in visual sensitivity. It is useful to show localized areas of sensitivity loss hidden within a field that is diffusely depressed.
For example, a person with dense cataracts may have decreased threshold across the entire visual field and this may obscure more focal losses due to coexisting disorders like glaucoma. Rather than comparing the patient’s threshold values with a normative database, the pattern deviation analysis finds the patient’s 7th most sensitive (85th percentile) non-edge point and gives it a value of zero
Each other test location is then compared with this value to correct for any generalized depression. It has been demonstrated that this method is the best for separating widespread or diffuse loss from localized loss.
The bottom-most probability plots are grayscale versions of the total deviation and pattern deviation maps. These maps may be useful to visually represent the statistical significance of the total and pattern deviation calculations. The grayscale maps should only be interpreted in conjunction with the numerical maps to avoid extrapolations.
On the right side of the printout are several useful numbers. The glaucoma hemifield test (GHT) compares groups of corresponding points above and below the horizontal meridian to assess for significant difference which may be consistent with glaucoma. Mean deviation (MD) is the mean deviation in the patient’s results compared to those expected from the age-matched normative database. T
his calculation weighs center points more highly than peripheral points. Pattern standard deviation (PSD) is a depiction of focal defects. It is determined by comparing the differences between adjacent points. Higher values represent more focal losses, while lower values can represent either no loss or diffuse loss.
Short-term fluctuations (SF) are a calculation portraying the variability between repeated measurements of the same test location. High SF decreases the reliability of the test. Corrected pattern standard deviation (CPSD) corrects the PSD for the SF. If there is high variability when testing the same point (high SF), PSD is given less weight due to decreased predictive value, and CPSD will therefore appear lower than PSD.
Along the bottom of the HVF printout is a gaze tracker. The patient’s pupil is monitored during testing, and each time the pupil moves (representing a loss of fixation or head alignment), an upstroke is recorded.
Losses of fixation decrease the accuracy of visual field testing because abnormalities will not correspond with the expected anatomic region of the retina and some may be missed entirely. When the gaze tracker loses view of the pupil (representing a blink or droopy upper eyelid), a downstroke is recorded. Pupillary obstruction can also decrease the accuracy of results.(ref)
Discover more from An Eye Care Blog
Subscribe to get the latest posts sent to your email.


You must be logged in to post a comment.